Local hospitals find benefits of robotic assistance in surgery
By Wendy Kilmer
Many Abilene area surgical patients are experiencing less invasive, less painful and more precise surgeries, often with shorter hospital stays and quicker recoveries as Abilene’s two major hospital systems have incorporated robots into their arsenal of surgical tools. ,In robotic surgery, or robotic-assisted surgery as it’s sometimes called, surgeons are equipped with high-tech devices that provide greater precision, smaller incisions and improved dexterity and movement compared to open surgery and laparoscopic surgery.
Both Abilene hospitals have robots that are used in several types of surgery. Abilene Regional Medical Center purchased its first robot in 2012, a four-pronged device used in urology, gynecology, and some general surgery. Hendrick purchased a similar but updated version of that robot with extra bells and whistles in 2016. And last year ARMC acquired a second surgical robot – one used specifically in orthopedic surgery.
Orthopedics

Melissa Livingston had never heard of robotic surgery, but she needed knee replacement and her situation was complicated by a previous car accident that required a plate and left her with a bowed gait. She was told traditional knee replacement would not be able to help her gait but a co-worker told her about a new surgeon in town who was trained in a robotic knee replacement option.
“I met with him and we talked about robotic surgery,” Livingston said. “I had never heard of it but I researched it online and after talking to Dr. Pitts, I decided to go that route, and it turned out wonderful.”
Dr. Todd Pitts came to work with Abilene Regional in September of 2017, after completing a year-long fellowship at the CORE institute in Phoenix, focusing on hip, knee and shoulder surgeries with an emphasis on robotic surgery.
“It’s relatively new in orthopedics,” Pitts said. “The first robotic total knee was done in 2016 at the CORE
institute while I was there. It was really cool to be involved in that first one.”
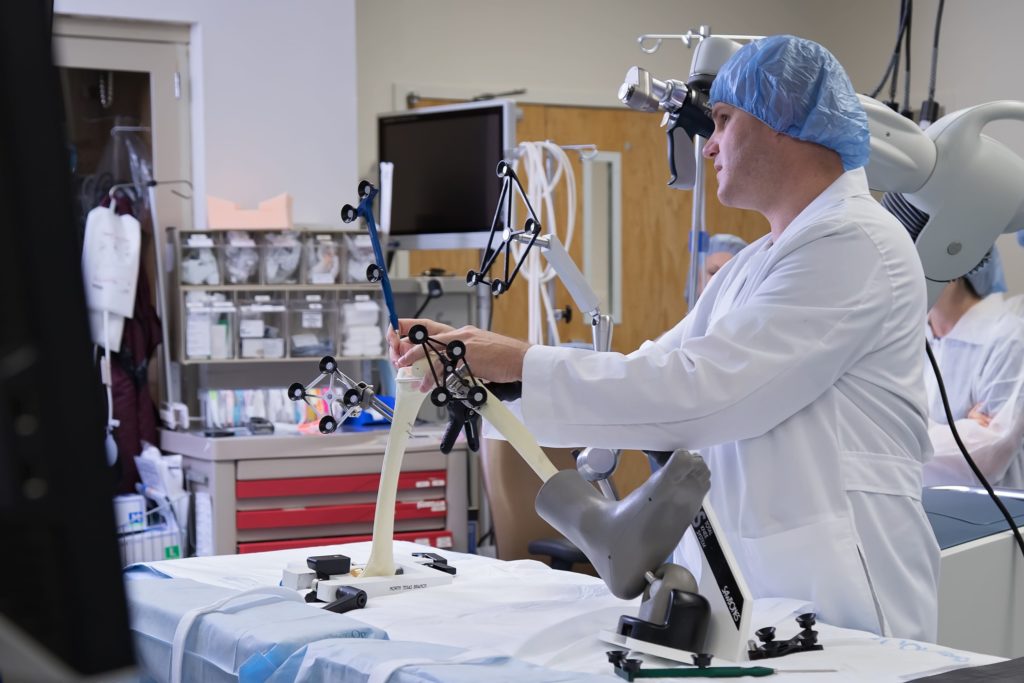
In such orthopedic surgeries, the surgeon, who is bedside and also working with a 3-dimensional image on a monitor, operates the single-armed robot directly. Much of the innovation takes place in the preparation for surgery. Patients undergo a CAT scan, and a 3D model of
the joint is created. Once in surgery, pins are placed that probe specific parts of the bone, and the 3D model on the screen is then synced with the actual knee.
“This allows me to make adjustments to the implant and how it fits before I make any cuts,” Pitts said. “Once we’ve fitted the implant, balanced it and rotated it to the right position on the 3D model, the hardest part of the surgery is done. After that, I guide the machine but the robot does the precise cuts. It’s on a fixed plane – the blade can’t deviate – so it protects patients.”
Thanks to this new level of precision in placement of the implant, fewer cuts have to be made to the bone, and implants are
balanced and fitted properly on the first try. Pitts likens advances in robotic technology to advances made in aircrafts back in the 1940s.
“I always say the idea behind it is the same argument made when planes changed instrumentation to become more mechanical,”
Pitts said “The pilot still can see and is involved, but so much more information can be assimilated through instruments. This is the same thing; it’s making knee surgeries better, more precise.”
Livingston found that to be the case. After being told by other physicians that her gait couldn’t be corrected, Pitts told her he
thought he could help. ARMC was still in the process of acquiring the new orthopedic robot in September 2017 when she first met with Pitts, but when it arrived, she was the first patient for robotic knee replacement in Abilene. Eighteen hours after surgery, she walked out of the hospital with a new knee and a straightened gait.
“I had been in so much pain with my knee,” Livingston said. “The surgery helped the pain and straightened my leg. I’m able to
do so much more now. And I hardly felt any pain afterward. The days the physical therapist came out were the only times I took pain medicine.”
Pitts said that’s not unusual. Patients often report less pain, shorter hospital stays and quicker recoveries through robot-assisted surgery. Physical therapists in town have told him they know right away which patients had their surgery done by him with the assistance of a robot – they’re the ones who are tempted to do too much, too quickly, because they have less pain.
Urology
Jeff Bell hadn’t heard of robotic surgery either, and it was not on his radar initially when he was told by Dr. Katherine Rinard, a
urologist at Hendrick, that his biopsy showed cancer in his prostate and a radical prostatectomy was needed.
“I didn’t know there was such a thing as robotic surgery,” Bell said. “I had family members who had that surgery done the old
fashioned way, and they had a big scar, and it was very invasive. But Dr. Rinard said ‘we’ve had really good success with this robot at
Hendrick doing this procedure.’
“I’m one of those guys who wants to know exactly what’s going to happen, and you know, you can find anything on YouTube, so I actually went on YouTube and watched a video of the surgery with this robot, and I thought ‘this is really cool.’”
Rinard came to Hendrick five years ago, and she was trained in robotic assisted surgery during her residency at Texas Tech University.
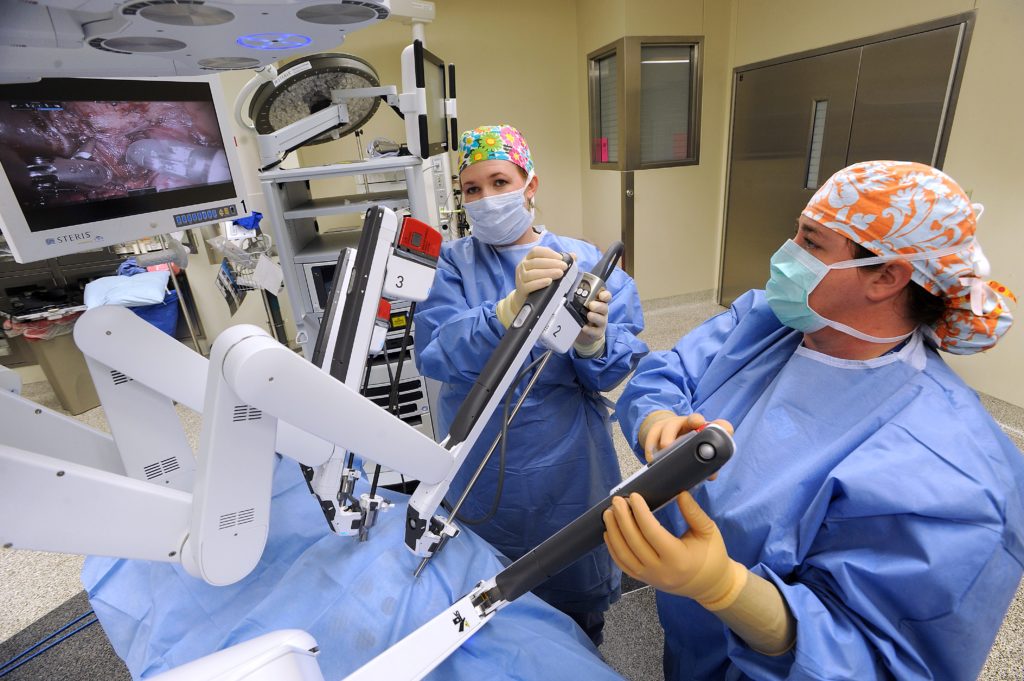
“When I came to Abilene, we didn’t initially have a robot, but I worked alongside several other surgeons as one of the early advocates of Hendrick acquiring it,” she said. “In the last 2-3 years, it has changed how we are able to do surgery. For patients, the advantages are less blood loss, smaller incisions, a shorter hospital stay and less pain after surgery. From a surgical standpoint, the advantage is in how the instruments move. Surgeons have a better visualization and a broader range of motion. It’s more technically precise. The difference between pure laparoscopic surgery, which is also minimally invasive surgery, and robotic-assisted laparoscopic surgery is like the difference between operating with instruments that move more like chopsticks versus using instruments that mimic human hand movements. This type of robot has four interactive arms that maneuver very small instruments and a camera. The arms are guided by the surgeon’s own hand and finger movements through a separate console nearby, yet they offer even greater dexterity and range of motion than a human hand and wrist.”
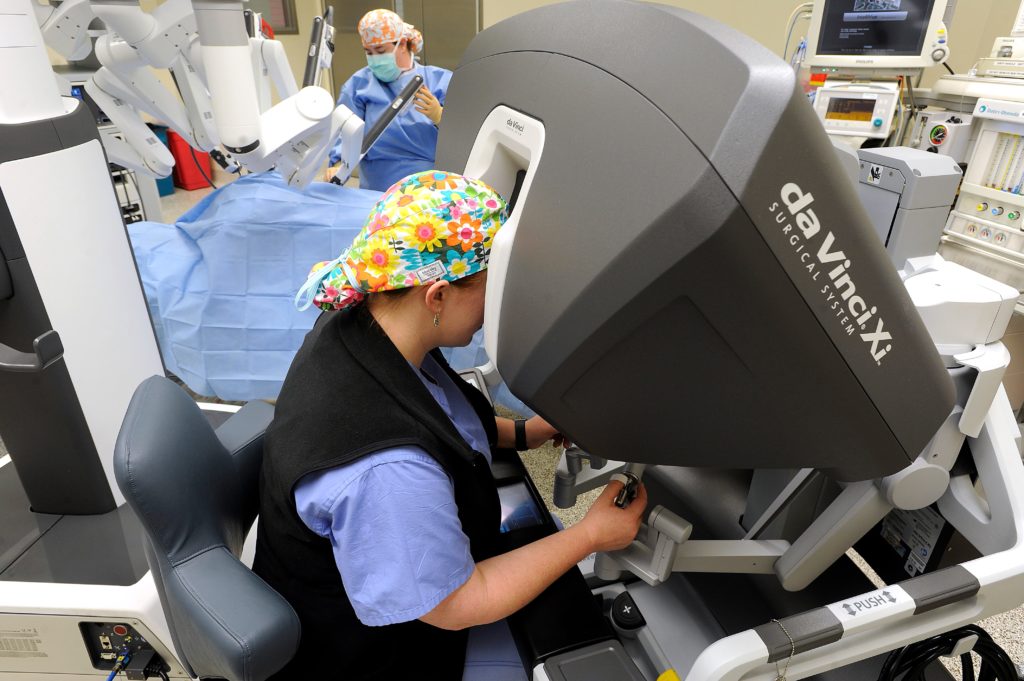
“The console has 3D vision and a small control panel where I see a high definition, 3D image and am controlling the robot’s movements,” Rinard said. “Surgical technicians assist with other instruments as needed. One of the concerns a lot of patients have is the idea of something robotic running on its own, but that’s not the case. I’m controlling the instruments, and I’m right there in the same room.”
The question Bell had for Rinard was “What if the machine breaks down right in the middle of surgery?” She assured him that it wouldn’t – and even if it did, she was fully capable of completing the surgery without it.
Bell was still awake when he was wheeled into the operating room and he remembers seeing the device.
“I was in awe,” he said. “It’s just a great technology. I got out of surgery about 9 a.m., and that evening I was up walking around the halls, and the next morning I left the hospital by noon. I never had pain medicine after leaving the hospital, other than Tylenol and ibuprofen. There was some soreness, but I was functional and mobile very quickly. The recovery was considerably faster than what it would have been with the old school procedure.”
Bell, owner of Pappy Slokum Brewery, did have to lay off lifting kegs for a few weeks but says he went in to work, made a batch of beer and could resume some parts of his work as soon as a week after surgery.
“I’ve become a big advocate for prostate health since then,” Bell said. ”And any time I can, I tell people about how cool this robotic surgery is too. Watching on YouTube, it’s amazing how delicate the procedure is. The robot can go from cutting to cauterizing a bleed as needed, and it’s so accurate and precise.”
Rinard says the most important part of the new technology for patients and families is how it affects outcomes, not just in
prostatectomies but in a variety of surgical situations.
“Ten to 15 years ago, an open nephrectomy might have meant a week in the hospital; now most of my patients go home just one day after taking a kidney out for cancer,” she said. “There is definitely less pain involved than open surgery, and there is even less pain between laparoscopic and robotic surgery although they use similar instruments.”
Gynecology
Dr. Nicole Bullock was a practicing obstetrician and gynecologist with Abilene Regional in 2012 when ARMC acquired its first robot. She took the hospital up on the offer to be trained to use the robot and was one of the first surgeons in Abilene to operate with it. She has been incorporating it into her practice ever since.
“It is a very minimally invasive surgery, and the post op recovery for patients is better. It’s just become the gold standard,” she said.
In her practice, hysterectomies are the most common robot assisted surgeries but it can also be used in removing ovarian cysts and fallopian tubes.
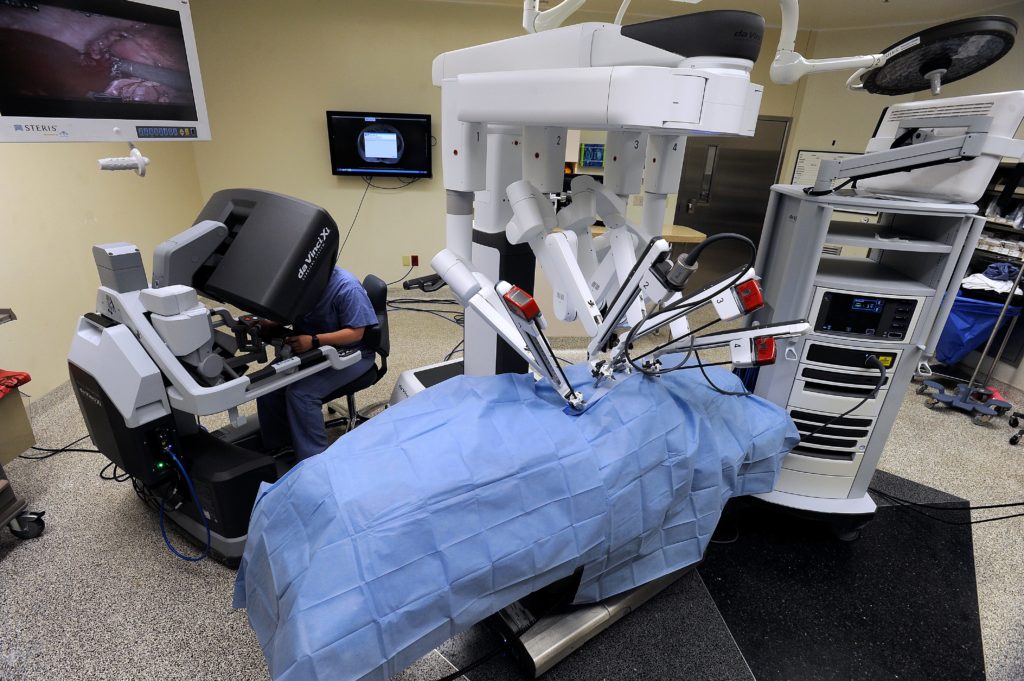
“The robot holds the instruments, which are docked over the patient, and the console is next to the patient,” she said. “I sit at the console and have amazing high definition, 3D visualization, and the fine motor control is amazing. It’s almost better than if I did a traditional open surgery. There’s 360 degrees of movement; the wristed joints give complete flexibility.”
A hysterectomy done with traditional open surgery would typically involve 2-3 days of hospital stay. With laparoscopic surgery, you’d stay overnight. With robotic you go home same day, Bullock said. “The post-op pain is incredibly minimal. Some go back towork in two weeks.”
The new technology has opened up new opportunities for collaboration in surgery. Recently Bullock took on a joint case with general surgeon Dr. John Cole. Cole was removing the gallbladder, and Bullock was performing a hysterectomy.
“I knew her ovary was pretty good sized, so when things are big, there can be adhesions, and things can be messier than expected,” Bullock said. “He did the gall bladder removal, saw some adhesions, removed those, and then realized the appendix looked inflamed, so he removed that too. Then I did the hysterectomy, and there was a lot of scar tissue. Then he came back to make sure there were no bowel injuries. We did keep her overnight, but she was just on oral pain medicine and two weeks later at her follow up, she was fine.”
Other types of surgery
Currently, four Abilene Regional surgeons (in gynecology and general surgery) use one robot, and another four surgeons use the orthopedic surgery robot. The robot at Hendrick is used by surgeons in colorectal, urology and general surgery.
Although some form of robotic surgery systems have been around for the past 18 years, initially they were larger and more cumbersome. Like many technological devices, advancements led to smaller, more streamlined products.
Dr. Leigh Taliaferro, general surgeon at Hendrick, began hearing about robotic surgery five or six years ago and was intrigued but didn’t think it was something he’d ever incorporate into his practice.
A conversation with a colleague at a Texas Surgery Society meeting a few years ago changed his perspective, however.
“A friend in Midland told me he starting using it and it was fantastic,” Taliaferro said. “And he is a good surgeon, so I thought I ought to look at it. I observed a few surgeries, then I trained on it, did a few cases, and now I’m an aficionado.”
Taliaferro most often uses the robot in hernia, gallbladder and colon surgeries where with the robotic device he can see better and has improved precision in sewing and dissecting.
“On top of that, it’s really improved how we make incisions,” he said. “They are less painful, and in today’s world of the opioid crisis, that’s important. Using the robot can mean less likelihood of prescribing narcotic medicine. Also with robotic incisions, they are so small; we hardly ever see a wound problem. With open surgery there can be complications with swelling, infection or fluids, and with robotic incisions we rarely see any of that.”
Colleagues also introduced Dr. Brad Kendrick, colorectal surgeon at Hendrick, to the benefits of robotic surgery.
“After hearing about results from other patients, and once I began doing it, it became obvious this would become the standard of care,” Kendrick said. “Before we acquired the robot, I had to send patients to Dallas for this type of surgery.”
Along with Rinard, Kendrick also was an early advocate for Hendrick to invest in the robot a few years ago.
“In today’s world, everyone coming out of medical school is trained on it in every specialty,” said Kendrick. “You have to have a robotic program that allows surgeons to access the robot. Patient care is so much better, there’s no reason not to. Better surgery, with better outcomes.”
Challenges and New Developments
New technologies naturally represent a significant investment for hospital systems. Surgical robots cost in the neighborhood of $1.5 to 2 million and incur additional costs for training, maintenance and future upgrades.
“Healthcare is very technology driven,” said Mike Murphy, CEO at ARMC. “There is always new stuff coming out. So what we have to do is ask ourselves ‘Is this the right technology at the right time for our patients in Abilene?’ And then, if it is, just like if you’re going to buy a car, you ask yourself more questions: ‘Do I buy now or wait? Should I buy or rent? Do I need the Lamborghini or will a Chevy work?’”
The purchase of a first robot in 2012 at Abilene Regional was initially driven by urology, Murphy said. Although they currently don’t have a urologist who uses it, they did at the time and Murphy anticipates they will again in the future. Having the robot available is important in recruiting physicians, particularly in high-demand specialties.
With the orthopedic robot purchased in 2017, the appeal was related to improved outcomes, Murphy said.
“Ultimately patient outcomes – less pain, less complications, quicker recoveries – those go into our decisions, as well as whether it is at least the same and maybe better for physicians,” he said.
Hendrick’s decision in 2015 to invest in the robot involved similar considerations.
“We examine the healthcare needs of the community, as well as the specialized training and staffing requirements prior to each technological purchase,” said Tracey Carrigan, director of surgical services at Hendrick. “Technological advancements and patient desire, as well as surgeon preference and industry standards, often dictate investments such as robotic surgery. We must also consider other issues including space allocation, staffing requirements, reimbursement and regulations.”
Future challenges and opportunities include investments in additional robots as demand increases, as well finding ways to increase the availability of robot and the necessary staff beyond daytime hours, potentially to 24-7 availability for surgeries.


























I’m interested on the topic of focusing on hip, knee and shoulder surgery. My dad may have to receive foot surgery soon, and I’m curious whether this could be applied to a minimal incision podiatric surgery. We’ll have to ask his doctor about this on the next visit.